Littmann CORE Sound Library: What You Can Hear Digitally (Heart, Lung, Bowel & More)
The Littmann CORE Digital Stethoscope extends traditional auscultation by adding digital amplification, noise reduction, recording, and waveform visualization, giving clinicians access to a clearer, more analyzable range of physiologic sounds. For many users, this effectively turns the CORE into a personal digital sound library, supporting faster recognition of subtle findings, improved diagnostic confidence, and better clinical documentation.
Unlike standard acoustic stethoscopes, the CORE allows clinicians to amplify soft sounds, filter background noise, and review or compare recordings over time using the Eko App. This makes it particularly valuable in busy clinical environments, during serial assessments, and when subtle changes matter. As an advanced electronic stethoscope, the CORE bridges traditional acoustic listening with modern digital analysis tools.
This guide outlines the types of heart, lung, bowel, and pediatric sounds clinicians commonly hear more clearly with the Littmann CORE, and why digital auscultation changes how those sounds are interpreted in practice.
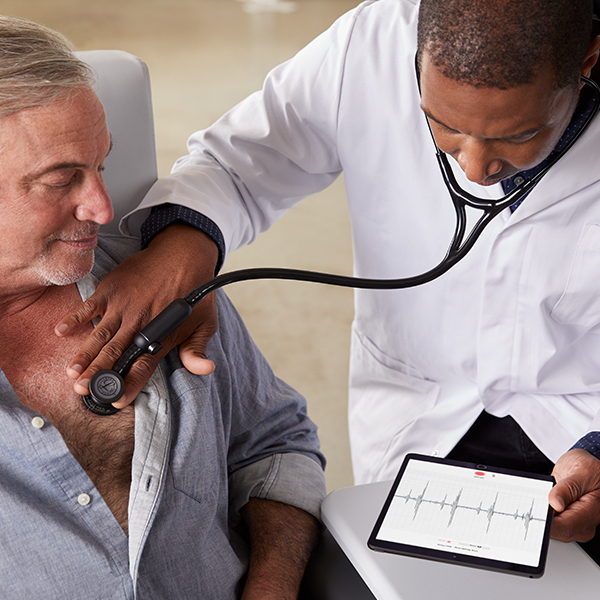
Why Digital Auscultation Reveals More Than Acoustic Listening
Digital auscultation is not about replacing clinical judgment; it’s about removing barriers that interfere with sound clarity. A high-performance digital stethoscope enhances sound detection by reducing the acoustic limitations that often interfere with subtle findings. The Littmann CORE enhances auscultation by:
- Amplifying low-volume and low-frequency sounds
- Reducing environmental noise that masks detail
- Allowing replay of findings for confirmation
- Providing waveform visualization for timing analysis
These capabilities are what distinguish a modern electronic stethoscope from a traditional acoustic device.
Through the Eko App, clinicians can record, store, and compare sounds, making it easier to evaluate progression, confirm subtle findings, or support communication with colleagues.
This functionality is especially useful for clinicians who:
- Work in noisy clinical environments
- Manage patients with subtle or evolving findings
- Perform serial assessments
- Support teaching, training, or case review
What Digital Amplification Can and Cannot Do
Digital auscultation enhances what you can hear, but it's important to understand the distinction between sound detection and clinical diagnosis.
What the CORE improves:
- Makes soft sounds louder and easier to hear
- Reduces interference from ambient noise
- Allows review and comparison of recorded sounds
- Supports documentation and teaching
What the CORE does NOT do:
- Replace clinical judgment or experience
- Automatically interpret abnormal sounds
- Guarantee accurate diagnosis
- Eliminate the need for pattern recognition skills
Critical distinction: Hearing a sound more clearly doesn't automatically mean you'll interpret it correctly. The CORE is a tool that enhances detection, but clinical interpretation still depends on your knowledge, experience, and overall clinical assessment. Like any advanced digital stethoscope, it improves clarity but does not replace clinical reasoning.
Think of it this way: amplification is like turning up the volume on a foreign language podcast—you'll hear the words more clearly, but understanding still requires language knowledge. Similarly, the CORE makes sounds more audible, but recognizing what they mean requires clinical expertise.
Heart Sounds: What the Littmann CORE Helps You Hear More Clearly
Cardiac auscultation benefits significantly from digital amplification, particularly for low-frequency or faint sounds that can be difficult to appreciate acoustically.
Normal Heart Sounds (S1 & S2)
The CORE improves clarity of timing and intensity of S1 and S2, making it easier to assess:
- Relative loudness
- Splitting patterns
- Subtle changes between exams
Waveform visualization supports confirmation of timing relationships when needed.
Additional Heart Sounds (S3 & S4)
S3 and S4 gallops are low-frequency sounds that are notoriously difficult to detect, even with amplification.
What the CORE offers:
- Improved low-frequency amplification may make these sounds more audible
- Noise reduction helps in loud environments
- Recording allows focused review
Realistic expectations:
- S3 and S4 remain challenging even with digital amplification
- Detection requires proper technique, optimal positioning, and clinical experience
- Amplification alone doesn't guarantee you'll hear subtle gallops
- Many factors affect detection: body habitus, lung interference, heart rate
Clinical perspective: While amplification helps, detecting S3 and S4 reliably requires significant clinical skill regardless of stethoscope type. Don't expect the CORE to make these sounds "easy" to hear, it simply improves your chances when optimal conditions exist.
Heart Murmurs
The CORE enhances murmur assessment by clarifying:
- Pitch
- Intensity
- Timing within the cardiac cycle
- Subtle changes with position or progression
Clinicians often find it easier to differentiate systolic, diastolic, continuous, and innocent murmurs, particularly in settings where ambient noise would otherwise interfere.
Clicks, Snaps, and Rubs
High-frequency transient sounds can be difficult to isolate acoustically. Digital amplification and noise filtering help highlight:
- Ejection clicks
- Opening snaps
- Pericardial friction rubs
- Mechanical valve sounds
These findings are often easier to confirm when recordings can be replayed or reviewed.
Lung Sounds: Where Digital Auscultation Shines
Respiratory sounds are frequently soft, fleeting, or masked by environmental noise, making them ideal candidates for digital enhancement.
Normal Breath Sounds
Digital clarity supports easier differentiation of:
- Vesicular
- Bronchial
- Bronchovesicular
- Tracheal breath sounds
This is particularly useful when comparing left-right symmetry or tracking changes over time.
Crackles
Fine and coarse crackles are often subtle and transient. The CORE’s amplification helps bring these sounds forward, making these sounds easier to hear when present. However, detecting crackles is only one part of respiratory assessment, clinical context, patient history, and other findings remain critical
Wheezes and Rhonchi
What amplification helps with:
- Distinguishing faint wheezes from background noise in loud environments
- Detecting subtle expiratory wheezing in patients with mild bronchospasm
- Hearing rhonchi when secretions are present but sounds are quiet
What amplification doesn't solve:
- Differentiating wheeze types (amplification doesn't change pitch characteristics)
- Determining severity (loudness doesn't always correlate with obstruction degree)
- Replacing spirometry or objective pulmonary function assessment
Practical note: Wheezes are often loud enough to hear acoustically. Digital mode is most useful when breath sounds are very soft or environmental noise interferes.
Stridor and Diminished Breath Sounds
High-pitched inspiratory sounds and areas or reduced airflow are easier to confirm digitally, particularly in:
- Pediatric patients
- Patients with obesity
- Settings where ambient noise interferes with acoustic listening
Bowel Sounds: Improved Confidence in Abdominal Assessment
Although bowel sounds are often quieter and inconsistent, digital amplification may improve detection of quiet bowel sounds:
- Hyperactive sounds
- Hypoactive patterns
- Borborygmi
- Absence of sound during focused assessments
It is worth noting that clinical decisions should never rely on auscultation alone. Consider patient symptoms, exam findings, and history. Recording can also be helpful when documenting findings or reviewing questionable results.
Pediatric Auscultation: Added Value of Digital Mode
Potential advantages in pediatric patients:
- Smaller chest pieces (CORE has pediatric side) improve contact on small chests
- Amplification may help with crying or uncooperative children
- Faster heart rates sometimes benefit from digital clarity
- Recording allows review after difficult examinations
Realistic challenges:
- Pediatric sounds are often already quite loud (less need for amplification)
- Movement artifacts increase with digital mode
- Children may be distracted or frightened by electronic sounds/lights
- Many pediatric abnormalities are easily heard acoustically
Evidence note: Limited pediatric-specific validation studies exist for digital stethoscopes. Most pediatric cardiologists still rely on acoustic stethoscopes for diagnostic assessments.
Best use cases:
- Noisy pediatric ED environments
- Teaching medical students or residents pediatric sounds
- Documenting findings for specialist consultation
- Home care or telemedicine pediatric assessments
Recording, Reviewing, and Building a Digital Sound Library
One of the CORE’s most impactful features is its ability to record and store sounds via the Eko App. This allows clinicians to:
- Compare findings over time
- Document subtle changes
- Review uncertain sounds
- Build personal or teaching sound libraries.
Waveform visualization further supports interpretation by clarifying timing relationships between sounds. This ability to create a personal archive of findings is one of the defining features of a modern digital stethoscope.
Clinical Evidence for Digital Stethoscopes
Research on electronic stethoscopes shows mixed but promising results:
Documented benefits:
- Improved sound amplification in clinical settings
- Enhanced ability to detect faint or low-frequency sounds
- Better performance in noisy environments compared to acoustic stethoscopes
- Useful for telemedicine and remote consultation via sound transmission
Current limitations in evidence:
- Most validation studies compare electronic vs. acoustic stethoscopes in controlled settings, not real-world clinical outcomes
- Limited research on whether improved sound detection translates to better diagnostic accuracy in practice
- Few studies examine impact on patient outcomes (earlier diagnosis, reduced complications, etc.)
- Optimal amplification levels for different conditions remain unstandardized
Bottom line: Digital stethoscopes like the CORE offer clear technical advantages (amplification, noise reduction, recording), but research on clinical impact is still evolving. Many clinicians report improved confidence and detection ability, though large-scale outcome studies are needed.
Sources: Studies on electronic stethoscope clinical utility have documented technical improvements while noting the need for more real-world validation research.
When Digital Auscultation Provides the Most Value
Based on clinical experience and user feedback, the CORE's digital features are most helpful when:
High-value scenarios:
- Extremely noisy environments (ED, ICU, field settings)
- Very soft or faint sounds that are barely audible acoustically
- Serial monitoring where comparison over time matters
- Teaching scenarios where sharing sounds helps learning
- Telemedicine consultations requiring sound transmission
Lower-value scenarios:
- Routine auscultation in quiet exam rooms
- Clear, loud, obvious findings
- When you already have high confidence in acoustic findings
- Quick screening assessments
Most clinicians report: Digital mode is used selectively (20-40% of assessments) rather than continuously, reserving it for challenging cases where amplification or recording adds meaningful value.
Frequently Asked Questions
Does digital auscultation detect more abnormalities than acoustic listening?
Digital enhancement often makes softer or low-frequency findings easier to detect, particularly in noisy environments.
Can clinicians share recordings with colleagues?
Yes. The Eko App allows secure sharing of de-identified recordings when clinically appropriate.
Does digital mode alter the natural sound?
No. Digital mode preserves the character of the sound while improving clarity and audibility, though amplification changes the relative loudness of frequency components, which can alter how sounds are perceived.
Is waveform visualization clinically useful?
Many clinicians find it helpful for confirming timing relationships and reviewing complex findings.
Can the CORE detect abnormalities I would miss with an acoustic stethoscope?
Sometimes, but not reliably. Amplification helps with very soft sounds, but most clinically significant findings are audible with good acoustic stethoscopes when proper technique is used. The CORE's main advantage is in challenging environments (noise, soft sounds, difficult positioning) rather than detecting entirely inaudible findings.
Will using the CORE improve my auscultation skills?
The recording and playback features can support learning by allowing review and comparison. However, developing auscultation skills still requires extensive practice, feedback from experienced clinicians, and exposure to many patients. The CORE is a tool, not a shortcut to expertise.
How accurate are the waveforms for timing analysis?
The waveforms provide useful visual representation of sound timing and can help clarify complex findings. However, they should complement, not replace, your auditory assessment. Waveform interpretation requires understanding of what you're looking at—it's not automatically diagnostic.
Do I need the CORE to hear most abnormal sounds?
No. The vast majority of clinically significant heart and lung findings are detectable with quality acoustic stethoscopes and proper technique. The CORE is most valuable for edge cases: very soft sounds, noisy environments, documentation needs, or when serial comparison matters.
Is digital auscultation replacing acoustic stethoscopes?
No. Acoustic stethoscopes remain the standard in most clinical settings. Digital stethoscopes are supplementary tools that offer specific advantages in certain situations but aren't necessary for most routine auscultation.